Melasma Treatment in London
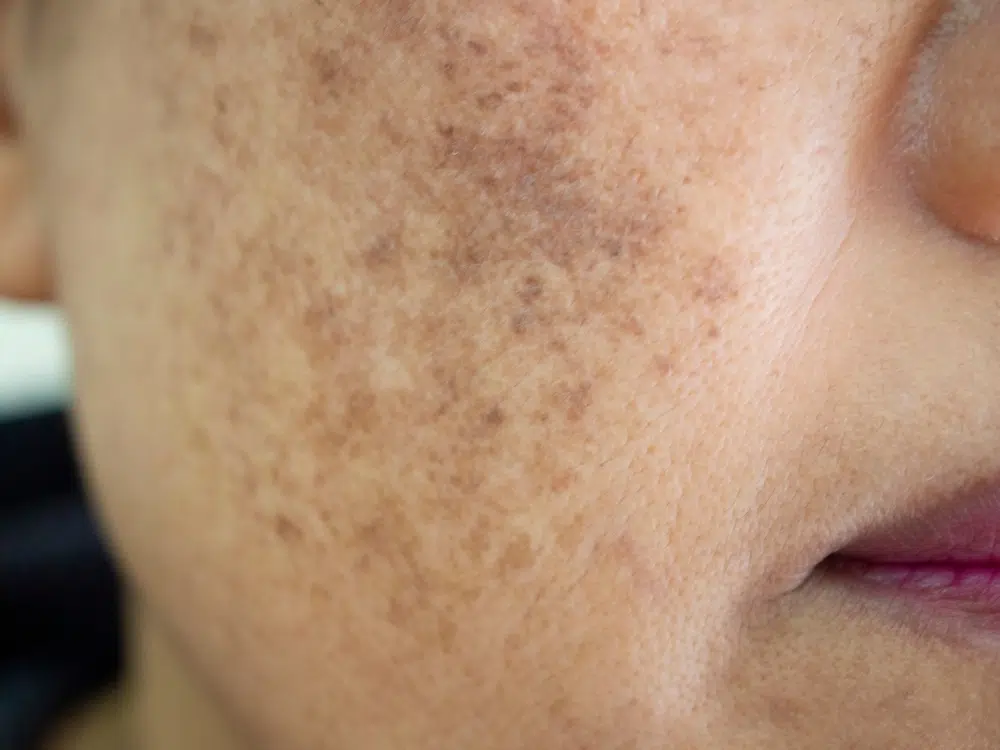
Melasma is a hyperpigmentation condition that impacts skin that is exposed to the sun. Melasma affecting the face is the most common type, and there are three known types of facial melasma – cheek, forehead, and melasma affecting the mandibular border. Melasma affecting the central part of the face is by far the most common subtype. The exact cause of melasma remains incompletely understood at the cellular level. There are several well-recognised causes of melasma or factors that predispose to its development, and these include UV sunlight exposure, hormonal influences and genetic factors. Although melasma is not a dangerous skin condition, it can cause enormous psychological upset and impact confidence and emotional well-being.
RELATED: Laser Pigmentation Treatment
Melasma most commonly affects women between the ages of 20 and 40 and mainly affects the facial region, particularly the forehead, cheeks, upper lip and nasal dorsum. Although melasma can occur at any time in life, it is most commonly precipitated by the hormonal changes that often occur during pregnancy. The influence of high circulating levels of certain hormones increases the likelihood of forming dark-pigmented skin lesions when exposed to direct sunlight, which contains ultraviolet radiation. Melasma can also develop in some cases from bright light from light bulbs over a sustained period. Melasma more commonly affects patients with darker skin types and is more likely to be seen in those of Asian, Middle Eastern, African or Hispanic origin. Melasma is significantly more common in women than men. Only approximately 10% of men develop some form of melasma hyperpigmentation.
Can melasma be treated?
The treatment of melasma is notoriously tricky. Our aesthetic practitioners and dermatologists have access to the full range of treatments to help improve the appearance of melasma. Still, it is essential to recognise that melasma cannot be fully cured. Melasma occurs very commonly during pregnancy but will often disappear entirely following childbirth after 3-6 months. Melasma may reappear during a subsequent pregnancy. At Centre for Surgery, our practitioners do not treat women who are pregnant or breastfeeding to avoid any risks to the mother and baby. Skin-lightening agents that are a common component of treatment for melasma include both skin-lightening and retinoid creams, and these must both be avoided completely when you are pregnant. Even with the most effective treatments, although they can significantly improve the appearance of melasma, recurrence is possible after stopping treatment or exposure to strong sunlight. Melasma is most effectively controlled when patients undertake a regular programme of preventive treatments, including medical-grade skin care products and certain laser treatments to control flare-ups.
What is Melasma?
Melasma is a common skin condition that primarily affects women, though men can experience it too. It manifests as patches of darker skin, typically appearing on the face. These patches, often brown or greyish in colour, are usually found on the forehead, cheeks, bridge of the nose, or the chin. In some cases, they may also appear on parts of the body that are frequently exposed to the sun, such as the forearms and neck.
The exact cause of melasma remains somewhat unclear, but several factors are believed to contribute to its development. Sun exposure is a significant factor, as ultraviolet (UV) rays from the sun can trigger melasma or worsen existing patches. Hormonal changes are also a key element, particularly those occurring during pregnancy, when melasma is commonly referred to as the “mask of pregnancy”. Additionally, birth control pills and hormone therapy can increase the risk of developing melasma.
Genetics play a role too, with a higher likelihood of melasma in individuals who have a family history of the condition. Skin type is another factor; those with darker skin are more prone to melasma due to having more active melanocytes, the cells responsible for producing melanin, the pigment that gives skin its colour.
Treating melasma involves a multifaceted approach. Sun protection is crucial, as UV exposure can worsen the condition. This includes wearing a high SPF sunscreen, seeking shade, and wearing protective clothing. Topical treatments, such as creams containing hydroquinone, may be prescribed to lighten the skin. Other options include topical steroids, tretinoin, kojic acid, or azelaic acid. Laser melasma treatment can also be considered, although its effectiveness can vary and they may not be suitable for everyone.
Living with melasma requires ongoing management, as the condition can be persistent and may recur, particularly if sun exposure is not adequately controlled. It’s important for individuals with melasma to consult with a skin care specialist at Centre for Surgery to determine the most appropriate treatment plan for their specific skin type and condition.
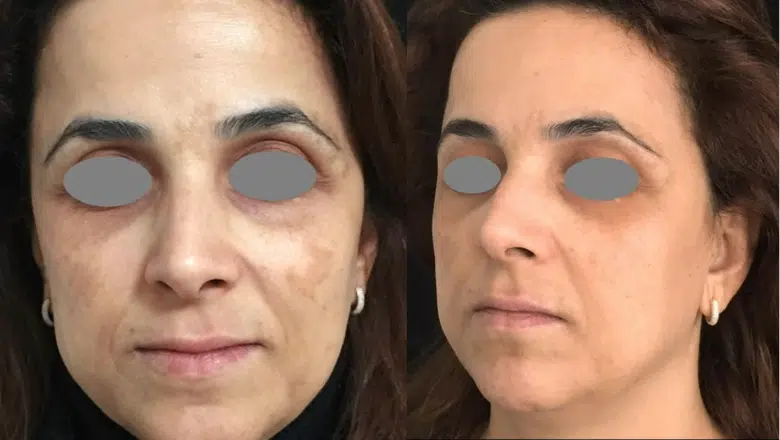
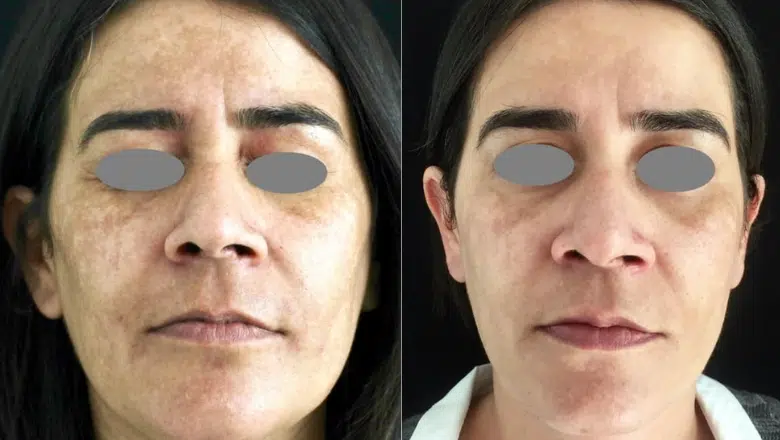
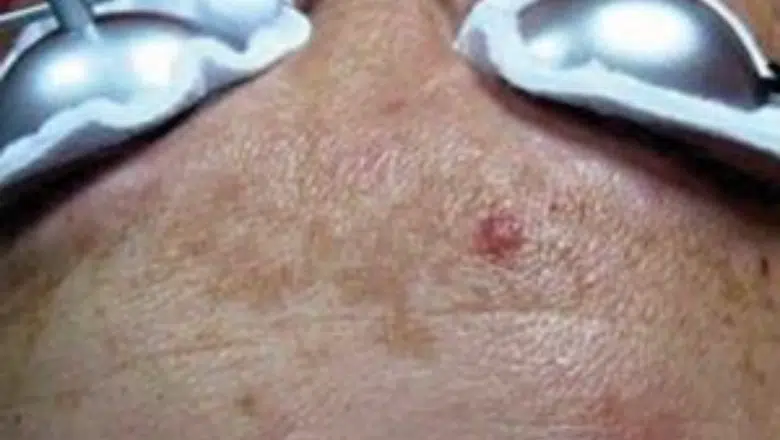
Melasma Laser Treatment Before & After
Causes of melasma
UV exposure
Ultraviolet radiation found in sunlight is a vital factor contributing to the formation of melasma in most patients. UV light can generate oxygen-free radicals and stimulate an increased production of melanin, which gives rise to the hyperpigmentation characteristic of melasma.
Hormonal factors
Hormonal factors play a crucial role in the development of melasma. There is a growing body of evidence which links the development of melasma with pregnancy, oral contraceptive usage and several other hormonal therapies or conditions.
Genetics
Although melasma is not a hereditary condition, several cases found in first-degree relatives have been described. Nonetheless, there is a genetic predisposition for darker skin types. Melasma mainly affects women, particularly those with darker skin types 3-6 on the Fitzpatrick scale.
Treatment options for melasma
The treatment of melasma is based on four key treatment approaches, which are more effective when combined.
Avoiding sun exposure and applying sunscreen
UV exposure is one of the leading causes of the development of melasma. Patients should take great care to minimise sun exposure to protect them from the effects of UV radiation, which is the cornerstone of treatment for melasma. It is well known that in the absence of proper sun exposure protection, melasma can recur, often in a more severe form.
Topical medications
Skin lightening creams: The currently available medical therapies are based on blocking the activity of the key enzyme tyrosinase, which is the main enzyme involved in melanin production. Although different drugs have been used for several years, there are no definitive guidelines on the best approach for medical treatment for melasma. Although short-term results can be excellent, long-term results can be less good as often has a tendency for relapse and/or recurrence. Skin lightening creams work to inhibit the action of tyrosinase enzyme and reduce melanocyte production. The effectiveness of topical creams is directly related to the concentration used, and the most commonly used formulation in the UK is currently 4%. There is a general agreement that above 4%, the irritant properties of skin-lightening cream outweigh the benefits of treatment.
Retinoids: Retinoids reduce melanin production through several pathways: firstly, they inhibit the transcription of tyrosinase. When used in combination with skin-lightening creams, it improves epidermal penetration. Published research has supported retinoids’ effectiveness in reducing melasma pigmentation subjectively and objectively.
Steroids: Although corticosteroids are known to have anti-inflammatory properties, they are not currently considered as a first-line agent for treating melasma as a standalone drug. There is an obvious concern regarding the well-known long-term side effects on the skin, including the development of acne and telangiectasia or thread veins. The main purpose of prescribing steroids is their role as a supportive agent in combination therapy treatments.
Azelaic acid: Azelaic acid is a tyrosinase inhibitor. It has the ability to destroy abnormal pigment-producing cells or melanocytes and reduce their activity.
Kojic Acid: Kojic acid has a dual action as a tyrosinase inhibitor as well as a potent antioxidant. It is much less effective than skin-lightening creams as a treatment used alone. However, it has been shown to have a benefit as a dual therapy when used in conjunction with other treatments.
Combination treatment
The purpose of combination therapy is to improve the effectiveness of a single agent and minimise the potential side effects of treatment. The Obagi Nu-Derm system is ideal for the treatment of melasma. Retinoids enhance the action of skin bleaching creams, which helps to improve the penetrative action through the skin’s epidermis and leads to a lower dosage requirement of medicines than when used singly. Steroids can potentially reduce the undesirable side effects of other agents. Combination therapies have been consistently shown to work quicker and more effectively than single agents because of the synergistic action.
Oral medications
The most commonly used oral medicine is tranexamic acid. Tranexamic acid is a well-known agent in surgery, where it is used to treat acute bleeding through the action of key reactants in the blood coagulation pathway. It inhibits the plasminogen activator, which ultimately inhibits the plasminogen’s transformation. Plasminogen can also be found in the skin cells or keratinocytes, as well as the basal layer of the epidermis. UV radiation has the ability to stimulate the keratinocytes/plasminogen system. This results in the production of prostaglandin and Leukotrienes. These two compounds are known to stimulate the production of melanin. The effect of tranexamic acid on binding to plasminogen in the epidermis will inhibit melanin production. Tranexamic acid may also increase the vascular blood supply through action on growth factors in the walls of blood vessels.
The effectiveness of Tranexamic acid in melasma has been widely studied and is used by dermatologists to treat melasma. Studies have shown that Tranexamic acid, in combination with topically applied creams and steroids, displayed a quicker response with longer-term remission compared to patients who do not receive the above combination.
Chemical peels and laser treatments for melasma
In-clinic treatments for melasma include dermamelan peels and laser treatments for reducing pigmentation and vascularity. Microneedling may also have a role in selected cases when combined with strict avoidance of sunlight exposure.
In-clinic treatments are usually combined with other first-line treatments, such as the Obagi Nu-Derm system containing skin-lightening agents and retinoids. Most studies support an additional beneficial treatment effect when combined with topical therapies. Laser therapy for melasma remains challenging, particularly in patients with darker skin types. In this particular group, which is known to be at a higher risk of melasma, laser therapy can generate side effects. Indeed, darker skin has larger and non-aggregated melanosomes. This higher concentration of melanin has the ability to absorb laser energy more diffusely and, therefore, trigger thermal lesions within the adjacent tissues. This can result in side effects such as post-inflammatory pigmentation and/or scarring. In addition, the melanin surrounding the area with melasma can act as a competitor (by absorbing the energy intended for melasma, hence decreasing the efficacy).
Ablative lasers such as CO2 and Erbium YAG lasers are not recommended for the treatment of melasma due to the substantial risk of inducing post-inflammatory hyperpigmentation. The most appropriate treatment is with a gentle non-ablative laser using Erbium Glass laser, often in combination with topical Tranexamic acid treatment and is safer to use in patients with darker skin types.
Melasma Treatment Near Me: Why Choose Centre for Surgery for Your Skin Care Needs
FAQs
-
What is melasma?Melasma, also known as ‘chloasma’ or ‘pregnancy mask’ is a hyperpigmentation skin condition that most commonly occurs in adult women. Brownish or grey patches of pigmentation develop on the skin and most commonly on the face. Melasma tends to occur most commonly in the summer months when sunlight is stronger and the skin has a greater sunlight exposure. Melasma is often much improved during the winter months.
-
Is melasma contagious?Melasma is a hyperpigmentation skin condition is not related to an underlying skin infection. It cannot therefore be transmitted from person to person.
-
Does melasma have the potential to develop into skin cancer?Melasma does not have any cancerous potential and is not related to to the development of skin cancer.
-
What are the causes of melasma?Although the exact cause of melasma is still incompletely understood, it is generally accepted that the condition is related to the stimulation of the melanocytes or pigment producing cells to produce the pigment melanin in excessive amounts.
Melasma is much more common in women than men especially when women become pregnant and melasma can affect up to 50% of pregnant women. Melasma more frequently affects individuals with darker skin types and also patients who have a propensity to tan very easily. Although melasma is not known to have a genetic basis, it is more commonly seen in patients who have an affected first degree family member.
Potential factors leading to melasma:
Hormone replacement therapy (HRT)
Oral contraceptive use
Pregnancy
Endocrine abnormalities that lead to oversecretion of certain hormones
Ultraviolet sunlight exposure
Regular sun bed use
Certain medicines such as drugs for epilepsy treatment